Fibromyalgia
Fibromyalgia
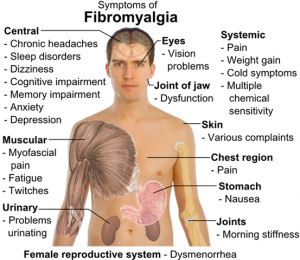
The most common symptom is widespread pain throughout the body, with especially tender spots near certain joints. The pain stops people with fibromyalgia from functioning normally, partly because they feel exhausted most of the time. Fibromyalgia is a chronic (meaning long-lasting) condition that usually requires many years of treatment. It can occur after an injury or out of the blue.
Pain in fibromyalgia is present in soft tissues throughout the body. Pain and stiffness concentrate in spots such as the neck, chest, shoulders, elbows, knees, buttocks, and lower back. The tender spots don’t seem to be inflamed. Most tests show nothing out of the ordinary in the anatomy of people with fibromyalgia.
The symptoms of fibromyalgia are long lasting and intense. However, they can vary from day to day. Some of the most common symptoms include
- pain and stiffness throughout the body, with especially tender points along the back of the neck, top of the shoulders, centre of the chest, elbows, knees, low back, and buttocks
- a feeling of exhaustion that sleep often does not help
- sleep problems
- tension headaches
- numbness or tingling in the arms and hands
- a feeling of swelling in the hands, although this is not confirmed in physical exams
- constipation and diarrhoea along with abdominal pain (known as irritable bowel syndrome)
- intense PMS pains in women
- depression
Causes
The causes of fibromyalgia are unknown, but one thing is for sure: you’re not making it up. Many sufferers have been told that it’s all in your head by family members or other doctors. It is true that people with fibromyalgia are often depressed, and that stress worsens symptoms. But depression and stress don’t seem to be the driving forces behind the disease.
Scientists haven’t been able to unlock all of the secrets behind fibromyalgia syndrome (FMS). Right now, the main theory is that FMS occurs when something goes hay wire in the nervous system. That something may be what’s called central sensitization syndrome. It means your nervous system is ramped up to react too soon, too often, and for too long.
New evidence suggests that fibromyalgia is really caused by a dysregulation of the central nervous system. There appears to be some kind of mistake within the nervous system in how it recognizes and transmits pain messages. Somehow, the nervous system seems to think even the simplest touch is a noxious (painful) stimuli. It’s like a ten-alarm fire signal is sent to the brain when a breeze blows by the barn. Nervous system dysregulation of this type is likely caused by biochemical abnormalities, altered brain blood flow, and problems with the pain processing mechanisms. Sufferers have lower pain thresholds and lower levels of serotonin, a brain chemical involved in pain, sleep, and mood.
Triggers
Folks who have fibromyalgia syndrome (FMS) often have certain triggers that seem to bring on (or increase) symptoms. The triggers vary from person to person but may include degenerative (spinal) disc disease, headaches (all kinds), irritable bowel syndrome, reflux (heart burn), trigger points of the muscles, and poor posture. Anxiety, depression, and post-traumatic stress disorder also seem to be linked with FMS.
Sleep
About 80 percent of all fibromyalgia patients report serious problems sleeping. Because fibromyalgia is so strongly connected to sleep disturbance, in some cases it is possible that the sleep disturbance may be a major contributing factor. In fact, studies have produced fibromyalgia-like symptoms in healthy adults by disrupting their sleep patterns.
Diagnosis
Primary or secondary
Sometimes FMS occurs as a result of an injury or some other medical condition. For example, patients with rheumatoid arthritis or Lyme disease (inflammatory diseases), metabolic dysfunction (e.g., thyroid problems), or cancer often develop a type of FMS referred to as reactive fibromyalgia. It’s important to identify whether or not the FMS is primary (the main problem) or secondary (caused by other problems).
Test
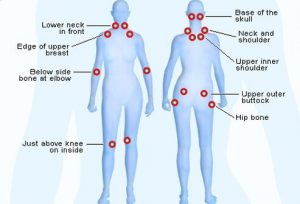
Blood tests and X-rays don’t show fibromyalgia in your body. However, your doctor may do these tests to rule out other conditions. Doctors have only two tools to diagnose fibromyalgia. One is your history of symptoms. The other involves putting pressure on eighteen tender point sites. If you feel pain in eleven of these eighteen sites, you are considered to have fibromyalgia. (However, it is still possible that you can have the disease with pain in fewer sites.)
Chronic fatigue syndrome (CFS) may need to be ruled out. CFS and fibromyalgia share many symptoms, especially the severe exhaustion. The major difference is that CFS causes flu-like symptoms, such as low-grade fevers, sore throats, and swollen lymph nodes.
Treatment
Today’s modern approach is multimodal, meaning many different treatment options are pursued at the same time. Combining medications with exercise, behavioral counseling, and alternative medicine have made it possible to live a more normal life for those who suffer with this condition.
All of the research so far confirms the need to treat this problem with a multidisciplinary approach. The treatments or lifestyle changes your doctor may recommend include
- exercise (aerobic and strength training)
- nutritional counselling
- massage
- acupuncture
- electrical stimulation
- behavioural cognitive therapy
- pain medication
Understanding
Usually the first step in the treatment of fibromyalgia is to help patients understand this complex and frustrating disease. Many patients are relieved to learn that the disease is not all in their head. After that, the task is to manage the pain and exhaustion.
Exercise
You’ll notice that exercise is listed first in the list above. That’s because there is a lot of evidence from good scientific studies that any form of exercise but especially isometrics (contract, hold, relax individual muscles) can be helpful. Pilates-based stretching, yoga, and low-impact aerobic exercise have the greatest benefit.
Anyone with fibromyalgia syndrome (FMS) must be very careful when trying weight-lifting, rowing, or jogging. In fact, these are not really recommended during painful flare-ups. Many people with FMS don’t have any real trouble during exercise. It’s the painful joint and muscle “after shock” that is the worst. Some can barely get out of bed the next day after what seems like a mildly strenuous work out.
Stretching exercises:
By increasing flexibility through stretching, tight, stiff muscles loosen up, providing relief. Your physiotherapist can instruct you on the proper way to stretch muscles, tendons, and ligaments.
Number of repetitions should be 5 to 10. Holding a stretch for 30 to 60 seconds is good for large muscle groups, with possibly only one or two repetitions necessary.

Aerobic exercises:
Low-speed and low-impact activities are best, stationary bicycles and elliptical machines are usually less stressful on the joints.

Aquatic exercises:
Swimming and other water exercises are excellent for patients with fibromyalgia. “The buoyancy of water can decrease the strain on muscles and joints and improve flexibility.” A heated pool can be especially beneficial because heat can soothe aching muscles.
Medication
Until the exact pathologic pathways are understood, treatment will be more of a management approach. The first-line treatment for fibromyalgia includes medications and a variety of other nonpharmacologic (nondrug) treatment. There isn’t one magic pill patients can take to wipe away the pain, improve sleep, or restore energy. Instead, a wide range of medications are available that can act on the nervous system in a variety of ways. These include tricyclic antidepressants, selective serotonin reuptake inhibitors (SSRIs), selective serotonin-norepinephrine reuptake inhibitors (SSNRIs), and anticonvulsants (also known as antiepileptics).
Neither one of these drugs seems to improve sleep. They do improve energy levels, physical functioning, and cognitive function — probably because they reduce pain, a symptom that can bring a person down in all these areas.
Pain relievers, whether over the counter or prescription, are generally not effective by themselves. Many pain medications are addictive and should be used with caution. Mild pain medications may help in combination with other treatments. Opioid (narcotic) pain relievers, corticosteroids, and nonsteroidal antiinflammatories (NSAIDs) are no longer recommended.
Massage
This can help muscle relaxation and stress management.
Nutrition
Eating a balanced diet can help provide better energy levels; it helps to maintain your weight, and gives you a greater sense of wellbeing.
Osteopathy Options for Fibromyalgia Relief
The increased flexibility and strengthen of muscles through an exercise routine are two important ways by which physiotherapy can help reduce fibromyalgia pain and make life more manageable.
Joint mobilization:
Can improve muscle tightness, tenderness and joint stiffness
TENS (Trans-cutaneous electrical nerve stimulation): TENS stimulates nerve fibers and can decrease fibromyalgia pain.
TENS helps:
- Block pain signals to the spinal cord
- Release the body’s own natural pain-killing chemicals
- Improve blood circulation and gently contract muscles for healing and relaxation

Soft tissue manipulation:
It is helpful in relieving muscle spasms or soreness, but is best used in combination with strengthening, stretching, lifestyle modification, and conditioning exercises.
Biofeedback:
Your physiotherapist might use biofeedback device that may help control muscle tension and reduce pain, and provide information about the amount of stress on your muscles.
The therapist places electrodes on the skin with a soft gel. This helps in recording the muscular tension. Your therapist can then explain how you can relieve that tension.
Sunlight exposure and fibromyalgia risk
There is no evidence that risk or symptoms of fibromyalgia are related to sunlight exposure.
Some people with fibromyalgia have a vitamin D deficiency. If so, vitamin D from solar ultraviolet-B (UVB) would reduce the symptoms.
Vitamin D and fibromyalgia
Vitamin D levels
Several studies report that people with fibromyalgia have lower vitamin D levels:
- In the United Kingdom, 43% of females with fibromyalgia had very low vitamin D levels compared to 19% without fibromyalgia.
- In Belfast, Northern Ireland, people with fibromyalgia frequently had low vitamin D levels. The study also linked anxiety and depression to low vitamin D levels.
However, other studies have different observations:
- In Israel and Brazil, vitamin D levels did not vary in people with or without fibromyalgia. In the same Brazilian study, there was no connection between vitamin D levels and pain intensity.
- In Turkey, neither vitamin D levels nor bone mineral density varied in people with or without fibromyalgia.
In all of the above studies, vitamin D levels could be the result of disease condition rather than the cause of the disease. Thus, the evidence that vitamin D plays a role in fibromyalgia is weak at best.
How vitamin D works
Some studies have reported that vitamin D may reduce the risk or symptoms of fibromyalgia by lowering inflammation. Vitamin D reduces cytokine production. This protein causes inflammation. However, one study found that fibromyalgia pain was not directly affected by these compounds.
Prevention
There is no evidence that vitamin D reduces the risk of fibromyalgia. However, it may reduce inflammation. Based on studies of other diseases, it might be worthwhile to keep vitamin D blood levels above 30–40 ng/mL (75–100 nmol/L).
Treatment
Vitamin D has been used to treat fibromyalgia in several studies and observations:
- In the United Arab Emirates, people diagnosed with fibromyalgia or muscle pain benefited from vitamin D. However, it was unclear whether those with muscle pain actually had fibromyalgia.
- People in Minnesota with fibromyalgia who initially had low vitamin D levels (10–25 ng/mL [25–63 nmol/L]) participated in a clinical trial. Some people received placebos. Others took 7000 international units (IU)/day of vitamin D3 (cholecalciferol). Vitamin D3 is the type of vitamin D made in the body. After 8 weeks, those receiving placebos showed no improvement. The vitamin D3 group showed significant improvement in fibromyalgia assessment scores. However, they did not show significant improvement in most musculoskeletal symptoms or in activities of daily living. In addition, those with severe vitamin D deficiency had no symptom improvement during the trial nor one year later.
- Diffuse back pain related to vitamin D deficiency is often diagnosed as fibromyalgia. Raising vitamin D blood levels reduces that type of pain.
Vitamin D may reduce fibromyalgia pain. Those with fibromyalgia should consider increasing their vitamin D levels above 30–40 ng/mL (75–100 nmol/L).
Prognosis
Patients do get better. In the ideal plan, the patient is really the manager who consults with these other experts to formulate the most effective plan. In fact, there is new evidence that half of all adults diagnosed with fibromyalgia early in the development of their disease (and who are adequately treated) no longer have this problem two years later. Many others have reduced their pain to tolerable levels.
Conclusion
Fibromyalgia is a general, debilitating disorder with widespread and fluctuating symptoms. It is important to recognise diagnosis, so that the patient has access to an appropriate therapeutic strategy.
Management of fibromyalgia is best carried out by using a multimodal and holistic approach with involvement of patient’s local doctor.
The patient themselves need to be encouraged to take an active role in their own treatment which augments any other therapeutic benefits.
Source:
www.eorthopod.com
www.healthclues.net
Colgan Osteopath in Kettering Northamptonshire
Colgan Osteopath in Hatfield, Hertfordshire
To book an appointment, call 07738493974 or book online