Hip Osteoarthritis
Colgan Osteopathy in Kettering and Hatfield
Hip Arthritis
Introduction
Osteoarthritis (OA) is a common problem for many people after middle age. OA is sometimes referred to as degenerative, or wear-and-tear, arthritis. OA commonly affects the hip joint. In the past, little was done for the condition. Now doctors have many ways to treat hip OA so patients have less pain, better movement, and improved quality of life.
Anatomy
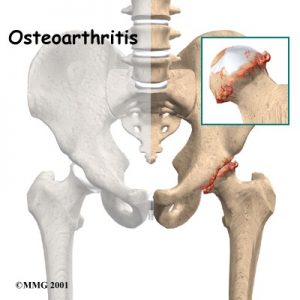
Articular cartilage is the smooth lining that covers the surfaces of the ball-and-socket joint of the hip. The cartilage gives the joint freedom of movement by decreasing friction. The layer of bone just below the articular cartilage is called subchondral bone. The main problem in OA is degeneration of the articular cartilage.
When the articular cartilage degenerates, or wears away, the subchondral bone is uncovered and rubs against bone. Small outgrowths called bone spurs or osteophytes may form in the joint.
Causes
OA of the hip can be caused by a hip injury earlier in life. Changes in the movement and alignment of the hip eventually lead to wear and tear on the joint surfaces. The alignment of the hip can be altered from a fracture in the bones around or inside the hip. If the fracture changes the alignment of the hip, this can lead to excessive wear and tear, just like the out-of-balance tire that wears out too soon on your car. Cartilage injuries, infection, or bleeding within the joint can also damage the joint surface of the hip.
Not all cases of OA are related to alignment problems or a prior injury, however. Scientists believe genetics makes some people prone to developing OA in the hip.
Scientists also believe that problems in the subchondral bone may trigger changes in the articular cartilage. As mentioned, the subchondral bone is the layer of bone just beneath the articular cartilage. Normally, the articular cartilage protects the subchondral bone. But some medical conditions can make the subchondral bone too hard or too soft, changing how the cartilage normally cushions and absorbs shock in the joint.
Avascular necrosis (AVN) is another cause of degeneration of the hip joint. In this condition, the femoral head (the ball portion of the hip) loses a portion of its blood supply and actually dies. This leads to collapse of the femoral head and degeneration of the joint. AVN has been linked to alcoholism, fractures and dislocations of the hip, and long-term cortisone treatment for other diseases.

Symptoms
The symptoms of hip OA usually begin as pain while putting weight on the affected hip. You may limp, which is the body’s way of reducing the amount of force that the hip has to deal with. The changes that happen with OA cause the affected hip to feel stiff and tight due to a loss in its range of motion. Bone spurs will usually develop, which can also limit how far the hip can move. Finally, as the condition becomes worse, pain may be present all the time and may even keep you awake at night.
Diagnosis
The diagnosis of hip OA starts with a complete history and physical examination by your doctor. X-rays will be required to determine the extent of the cartilage damage and suggest a possible cause for it.
Other tests may be required if there is reason to believe that other conditions are contributing to the degenerative process. Magnetic resonance imaging (MRI) may be necessary to determine whether your hip condition is from problems with AVN.
Blood tests may be required to rule out systemic arthritis or infection in the hip.
Treatment
Nonsurgical Treatment
OA can’t be cured, but therapies are available to ease symptoms and to slow down the degeneration of the joint. Recent information shows that your condition may be maintained and in some cases improved.
Your physician may prescribe medicine to help control your pain. Some people may also get relief of pain with anti-inflammatory medication, such as ibuprofen and aspirin.
Medical studies have shown that glucosamine and chondroitin sulfate can also help people with OA. These supplements seem to have nearly the same benefits as anti-inflammatory medicine with fewer side affects. Many doctors feel the research supports these supplements and are encouraging their patients to use them.
If you aren’t able to get your symptoms under control, a cortisone injection may be prescribed. Cortisone is a powerful anti-inflammatory medication, but it has secondary effects that limit its usefulness in the treatment of OA. Multiple injections of cortisone may actually speed up the process of degeneration.
Repeated injections also increase the risk of developing a hip joint infection, called septic arthritis. Any time a joint is entered with a needle, there is the possibility of an infection. Most physicians use cortisone sparingly, and avoid multiple injections unless the joint is already in the end stages of degeneration and the next step is an artificial hip replacement.
Physical therapy plays a critical role in the nonsurgical treatment of hip OA. A primary goal is to help you learn how to control symptoms and maximize the health of your hip. You will learn ways to calm pain and symptoms, which might include the use of rest, heat, or topical rubs. A cane or walker may be needed to ease pressure when walking. Range-of-motion and stretching exercises will be used to improve hip motion. You will be shown strengthening exercises for the hip to steady the joint and protect it from shock and stress. Your therapist can suggest tips for getting your tasks done with less strain on the joint.
Nonsurgical Rehabilitation
Nonsurgical rehabilitation of hip OA is used to maximize the health of your hip and to prolong the time before any type of surgery is necessary. If you attend physical therapy as part of nonsurgical rehabilitation, you will probably progress to a home program within two to four weeks.
In cases of advanced OA where surgery is called for, patients may see a physical therapist before surgery to discuss exercises, special precautions to be followed just after surgery, and to practice walking with crutches or a walker.
The therapist’s goal is to help you maximize hip strength, restore a normal walking pattern, and do your activities without risking further injury to your hip. When you are well underway, regular visits to the therapist’s office will end. Your therapist will continue to be a resource, but you will be in charge of doing your exercises as part of an ongoing home program.
Alignment
Muscle strength to improve shock absorption
Prevalence of abnormal hip findings in asymptomatic participants: a prospective, blinded study
https://pubmed.ncbi.nlm.nih.gov/23104610/
Colgan Osteopathy in Kettering Northamptonshire
Colgan Osteopathy in Hatfield, Hertfordshire
To book an appointment, call 07738493974 or book online